The omicron variant of the coronavirus has caused case counts to explode across the nation and globe since its discovery shortly after Thanksgiving. Early data on the variant shows it may be easier to transmit and have an increased ability to evade immunity from either prior infection or vaccines.
The surge has left many people wondering how they can protect themselves, or if infection is inevitable. Dr. Bisola Ojikutu, head of Boston Mayor Michelle Wu’s COVID-19 Advisory Committee, and Dr. Cassandra Pierre, medical director of Public Health Programs at Boston Medical Center,joined Greater Boston on Thursday to encourage people not to throw in the towel.
Is it inevitable that we are all going to get omicron?
Infection is preventable with vaccines, boosters, well-fitting masks and rapid antigen testing, according to Ojikutu.
“I wouldn't give in and say ‘Oh, we're all going to be infected.’ I would say that we should implement the mitigation strategies that we know are evidence based and do them on a regular basis," she said. "And I think that many people will not be infected necessarily with this variant or any other.”
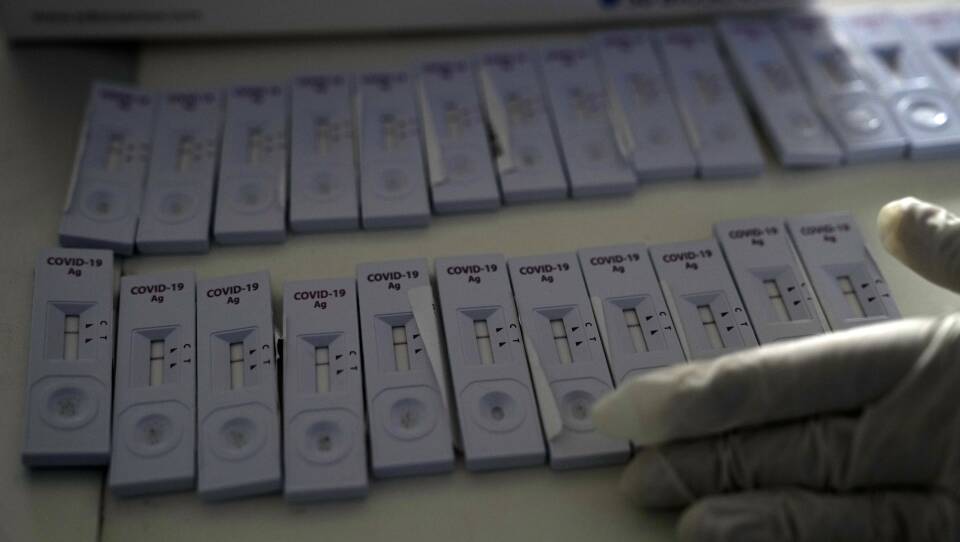
Can the rapid home tests detect this variant?
The Food and Drug Administration has been collaborating with the National Institutes of Health to study rapid antigen tests on the market and their ongoing performance. That research indicates that while at-home tests are able to detect the omicron variant, they may have reduced sensitivity, meaning the tests might be more likely to show a negative result for patients who are infected.
Generally, rapid antigen tests are less sensitive than molecular (PCR) tests. If you have symptoms or a high likelihood of infection because of a known exposure, the FDA recommends following up a negative home test with a PCR test.
The FDA also identified PCR tests that are unable to detect the omicron variant: Meridian Bioscene’s Revogene test and Applied DNA Sciences’ Linea test.
Should I just get coronavirus now so I can have immunity and avoid getting sick later?
“Even if you believe this is [an] inevitability, we should not let this wash over us. I definitely disagree with getting it now versus later,” said Pierre.
There’s also basic math at play. More cases overall, even mild ones, mean more people are able to spread the virus — in turn leading to more severe disease and deaths.
"So in a crowded, overtaxed healthcare system where it might be difficult to even access tests, might be difficult to access treatment, this is not the time to get sick," Pierre said.
How long after exposure does it take for a person to get sick?
The omicron variant appears to make people sick faster than previous variants. The incubation period for the original strain was more than five days, and the delta variant was about four days. Omicron, however, showed up after a median of three days among family members in a small study by the Nebraska Department of Public Health and reviewed by the CDC.
How can I tell the difference between cold symptoms and omicron?
Coronavirus symptoms, including symptoms of omicron, often overlap. Such overlapping symptoms include congestion and runny nose, sore throat, coughing and fever, according to the CDC.
However, some symptoms stand out. Coronavirus symptoms that differ from colds include chills, shortness of breath, body aches, loss of taste or smell, nausea, vomiting and diarrhea.
Cold symptoms that differ from coronavirus symptoms include sneezing, post-nasal drip and watery eyes.
How is omicron impacting public health?
Patients are forgoing, delaying or rescheduling treatments, surgeries, screenings and preventive check-ups which lead to bigger and more severe consequences, Pierre said.
“In the past few months more people are presenting with more progressed malignancies, cancers, people coming in with new or worsened in cases of diabetes — so many things that while not directly attributable to the virus, have been worsened by people’s inability to get into health care,” Pierre said.
WATCH: Can we get the COVID-weary to care about safety again?